When I was first diagnosed with IBS back in 2008 I was having an incredibly hard time controlling my symptoms even with the recommendations from my Doctor. So, like you, I turned to the internet for answers. I spent hours scouring the internet for information on how to control or even get rid of IBS. I read everything: forums, blogs, and those questionable Yahoo answers (does Yahoo even exist anymore?! Am I aging myself there?).
I was desperate for information. I also became fixated on the idea that there was one magical cure out there-whether it be a supplement or a specific food- and, if I only searched long and hard enough, I would find it and end my struggle with IBS, forever.
Honestly, I tried everything. Many of them actually made my symptoms worse (with colon hydrotherapy being the worst offender) and I wasted thousands of dollars in the process.
Keep in mind that this was before the wonderful research that has been done around IBS so we now have a much better understanding of what causes IBS.
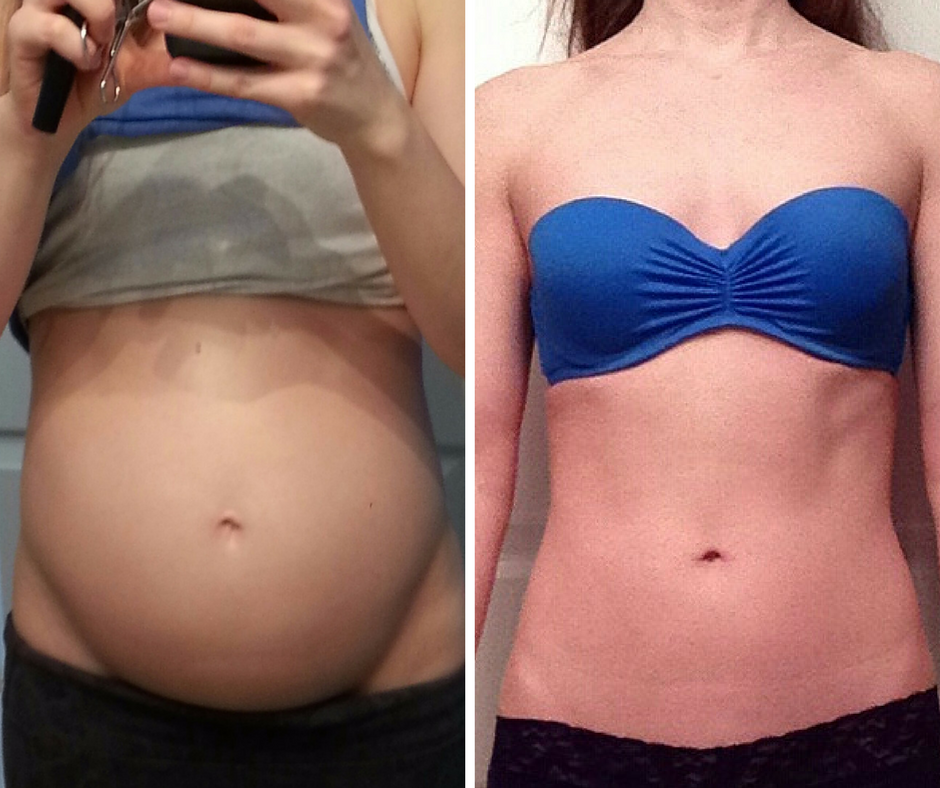
Over time and after much trial and error, I came to realize that it would take a holistic approach to control my IBS symptoms. I had been looking for a magical cure but what I really needed to focus on was my nutrition, my lifestyle and my mental well-being. After dedicating time to these areas, I was finally able to break free from the discomfort of IBS. Here is what helped me the most:
1) I went through a Low FODMAP elimination diet
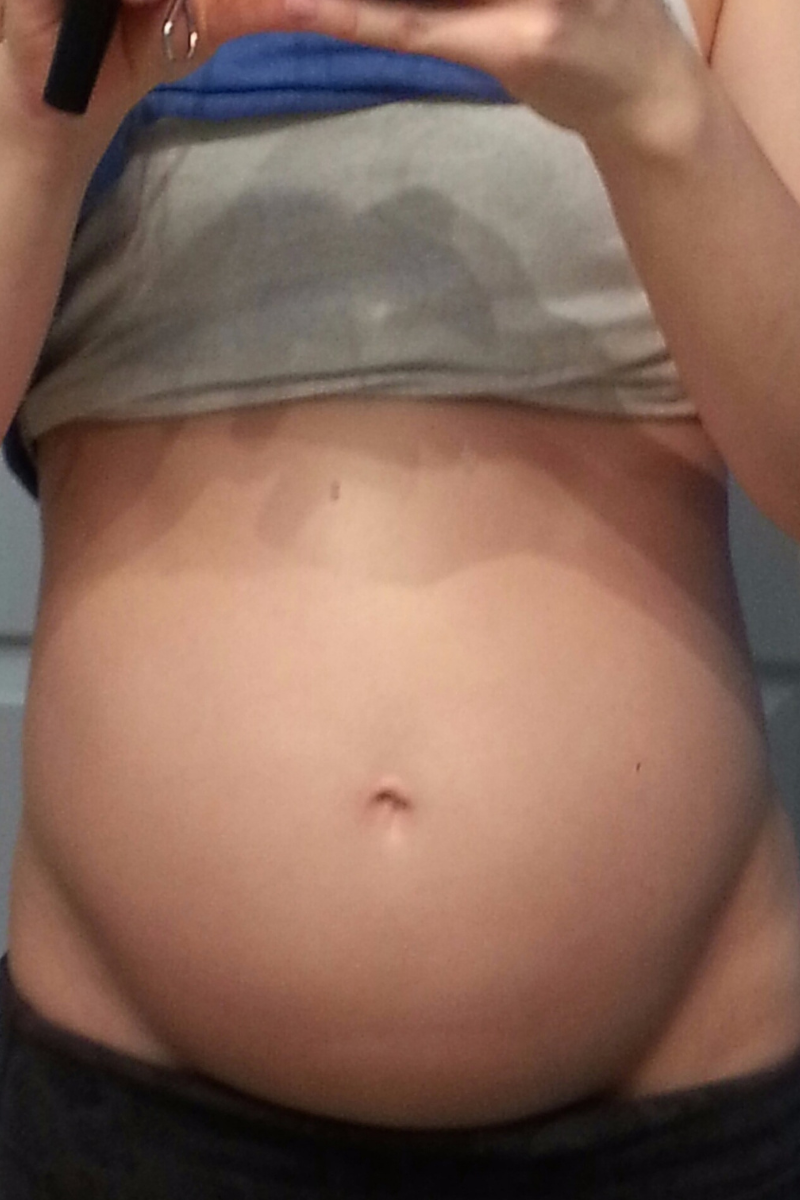
FODMAPs are a group of carbohydrates found in everyday foods like apples and garlic that some people are unable to digest. Two things can happen when eating FODMAPs: they have an osmotic effect and water is drawn into the intestines or they are highly fermented by bacteria in the intestines. Both result in IBS symptoms: gas, bloating, distension, constipation and/or diarrhea.
Reducing FODMAPs in your diet therefore reduces these symptoms. This was discovered by the research teams at Monash University who developed a Low FODMAP diet as a way to reduce IBS symptoms through diet. It remains the most effective dietary approach to controlling IBS.
A Low FODMAP diet is an elimination diet that removes high FODMAP foods for 2 – 6 weeks. Once symptoms have reduced, you then strategically reintroduce FODMAP groups to assess your tolerance. From there, your diet is customized to allow as many high FODMAP foods that you can tolerate. It takes time and patience to go through the reintroduction period but it is essential for your long-term gut health. Staying on a low FODMAP long term can reduce the amount of good bacteria in your gut- the opposite of what we want to do with grumpy guts!
After following the Low FODMAP diet followed by the reintroduction period I now know what foods cause symptoms for me and how much I can and cannot tolerate. This has allowed me greater freedom with my diet rather than what people often do: stick with an incredibly small list of foods that they tolerate and feel burnt out with their diet.
Curious about the Low FODMAP diet? You can download my Ultimate Debloat Meal Plan for IBS here.
2) I nourished my gut microbiome
The gut is home to an ecosystem of microbes that are responsible for many aspects of good health including the immune system, digestion and vitamin synthesis. Research even shows that our gut microbiome influences our weight! Dysbiosis – the term used to describe a change in the gut microbiome- is an underlying reason why IBS can develop. Dysbiosis can look like: too little “good” bacteria, infection by a parasite or “bad” bacteria, bacteria that has migrated to the small intestine (SIBO) or fungal overgrowth.
I had to address SIBO and fungal overgrowth to improve the health of my gut microbiome. This process is a whole blog post on its own but the short version looked like reducing bacterial and fungal microbes through antimicrobials, adjusting the diet to reduce fermentable carbohydrates (FODMAPs) and sugar and eating a variety of tolerated plant-based foods to help “good” bacteria grow.
I continue to eat a whole foods diet with a variety of fibres that help good bacteria thrive.
3) I learned how to better control my anxiety
The Enteric Nervous System (the “ENS”) plays a huge role in IBS. The ENS is the nervous system that resides in your gut. It regulates digestion and is in constant communication with the Central Nervous System (the “CNS”). Getting butterflies in your stomach when you feel nervous: that is the CNS and ENS communicating with each other.
In IBS, there appears to be a feedback loop between the CNS and ENS that is “misfiring” and causing intestines to speed up too fast or slow down too much. If you are an inherently anxious person (like me) or have major stressors in your life, you will need to put more focus on the ENS to control IBS symptoms.
This will look very different for everyone. You may need to make changes on a smaller scale like getting an extra hour of sleep each night. Some people need to make large-scale changes like switching careers or leaving dysfunctional relationships. Personally, this is how I have reduced anxiety:
- I worked with a Registered Counsellor who used CBT and talk therapy to help me overcome patterns of thinking that were intensifying anxiety.
- I keep my blood sugar balanced by eating balanced meals/snacks at regular intervals throughout the day. Do not underestimate the power blood sugar has over anxiety. I can be reduced to a puddle of tears and despair just from not eating or eating too much sugar.
- I broke my habits of being an overachiever and perfectionist. Counselling also helped with this. Any other Type As with me?
- I have solid boundaries around commitments and self-care. Self-care for me looks like 8 hours of sleep every night, exercising three times weekly, eating well and having lots of alone recharge time…and I stay committed to this even if it means cutting back on my workload or saying no to things.


+ show Comments
- Hide Comments
add a comment